Ask Rebecca Niziol, 34, about life before Lyme, and she remembers bounding around with infinite energy. A life coach and yoga instructor, she packed her schedule with hikes, Pilates workouts, client calls, meet-ups with friends, and weekend getaways. Then, in July 2020, she felt something change.
It started with neck pain and headaches. At first, she brushed them off as side effects of sitting in a car for hours on a road trip from Chicago to Colorado to visit family. Over the next few weeks, though, she continued to develop flu-like symptoms. It was the early months of the pandemic, so her immediate thought was COVID. But tests kept coming back negative.
She couldn’t practice yoga for a month. “I was in bed 20 hours a day,” she says. Her doctor suspected loneliness and pandemic-related anxiety, but her gut told her this was different. Something more physical, never-ending. She wouldn’t learn that she was battling Lyme disease for more than a year, when she connected with a “Lyme-literate” doctor and her labs confirmed it.
More From Women's Health

Brittany Barry, of Utah, faced a similarly confusing crisis last summer. Given that she was a self-described “healthy, fit, 32-year-old woman” at the time, doctors chalked up the muscle aches, fatigue, and shortness of breath to long COVID—a term for the phenom of health problems continuing long after someone tests positive for the virus. (She had COVID in February 2021.) One MD blamed post-pregnancy changes, while another told her to see a counselor.
Fast-forward to January 2022, when she found a doctor who did blood work that pointed to Lyme that had likely gone undetected for years.
Parallel Experiences
A coincidence that these women’s diagnoses came when they did? Maybe. But just like Niziol and Barry, many who’ve been impacted by long COVID, Lyme, or even both in the past few years are realizing they’re telling a similar story. There’s been a shift in empathy for chronic-illness and autoimmune patients who are stuck in a cycle of nonspecific symptoms that medical experts don’t totally know what to do with, says Niziol, who is still managing Lyme today.
Despite many yet-to-be-solved mysteries (we’ll get into those!), physicians and patients alike can agree the suffering is real—as is the serious change in perspective, says Robert Kalish, MD, a rheumatologist and the director of the Lyme Disease Clinic at Tufts Medical Center. “The pandemic helped people grasp the idea that you can get an infection, kill the initial cause, and still suffer lasting consequences from damage that’s been done—even if it’s difficult to detect or understand,” he says.
When you’re sick, you crave validation. Recognition gives you a better chance at care, not to mention dignifies your reality. “There’s a lot of similarity in experience between long-haulers and folks with chronic illnesses like mine being misunderstood or misdiagnosed,” Niziol says. “I might not have what you have, but I relate and deeply empathize.”
Diagnosis Dilemma
More compassion is huge. But it doesn’t erase the fact that Lyme is the most common tick-borne infection in the U.S., with an estimated 476,000 new cases each year (although only an estimated 35,000 get reported annually because of how difficult it is to diagnose). Since 1991, the prevalence of Lyme has nearly doubled as deer ticks, the main carriers of the disease, have expanded their territory. What’s more, increasing temps are expected to up Lyme cases by more than 20 percent between 2036 and 2065, a recent study found.
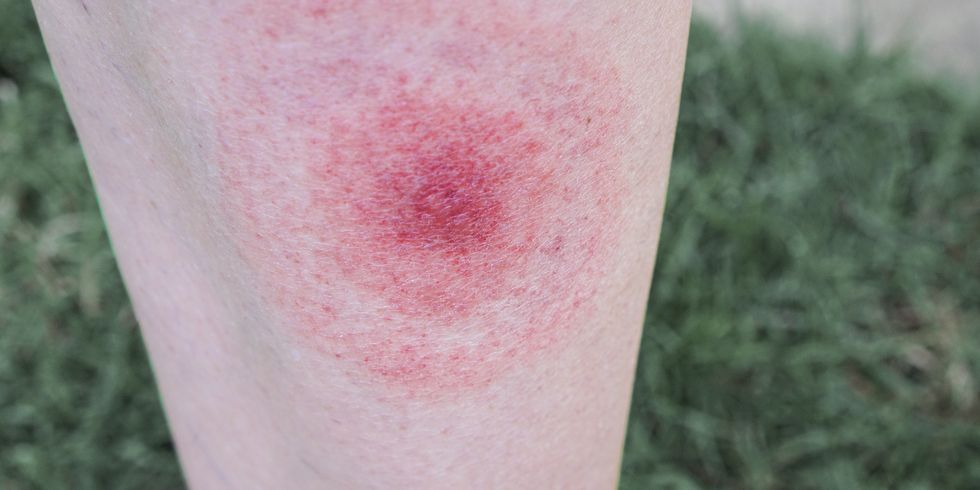
So, yes, a very real and growing threat, yet Lyme has been steeped in controversy pretty much since it was discovered in the ’70s. For one thing, there’s no perfect test: False negatives and positives happen often, which makes getting a correct diagnosis a challenge. Not every positive person shows the one telltale symptom—a bull’s-eye–shaped rash—either. (Niziol and Barry have no recollection of one.)
Further complicating the path to an accurate diagnosis is that Lyme, nicknamed “the great imitator,” can look like a bunch of other conditions, such as multiple sclerosis, depression, fibromyalgia, or a general viral infection. Niziol faced multiple misdiagnoses as her symptoms escalated to brain fog, blurry vision, bouts of numbness in limbs, and gaps in memory, as the months rolled on without answers. “I felt like a shell of a human,” she says. “My vibrancy was gone; joy left my body.”
Long-Haul Life
If and when you get a definitive read? The fight doesn’t necessarily stop there. With speedy detection and treatment (typically a four-week or longer course of antibiotics), the infection is usually easy to resolve at first. But for many, including Niziol, symptoms live on.
In August 2021, just over a year after her symptoms first emerged, and still desperate to find a doctor who really understood, she searched online for specialists in her area. This time, she visited Casey Kelley, MD, a family and integrative medicine physician. Dr. Kelley ran a slew of tests and diagnosed Niziol with chronic Lyme. (Just when you thought things couldn’t get trickier!)
The diagnosis most commonly given is post-treatment Lyme disease syndrome, or PTLDS. But some doctors go so far as to use the term “chronic Lyme disease,” though this is not a diagnosis recognized by the National Institutes of Health. That’s because in one camp, you have pros who question the legitimacy of this term that indicates an ongoing infection, citing human studies that show meds are effective in killing bacteria that cause Lyme. On the other side are docs like Dr. Kelley who believe chronic Lyme is real even if it’s unclear why it happens. (She points to studies that suggest a long-term infection remains.)
Whatever you call it, “This much is not controversial: There’s no proven effective treatment for persistent Lyme,” says Linden Hu, MD, a professor of immunology at Tufts University School of Medicine. Depending on your doctor, solutions could involve meds, supplements, and/or an anti-inflammatory diet. “A two-steps-forward, one-slide-back kind of situation,” Niziol says.
Health On The Horizon
The reassuring news is that real advancement is underway. In the past few years, tens of millions of dollars have been dedicated to combating Lyme. Researchers at Columbia University are working on brain imaging studies to better understand symptoms like chronic fatigue and pain that come with the infection.
Game-changing innovations to defeat the disease are also in the pipeline. A vaccine being tested in guinea pigs (thank you, Yale researchers) triggers an immune reaction to a tick bite that helps get the bug to detach, inhibits its ability to feed from you, and reduces transmission of the pathogen. Another candidate, from Valneva and Pfizer, works by killing bacteria in the bloodsuckers. Early studies indicate the prick is safe, and you might be able to get it as soon as 2025.
Researchers at Tufts University also set the lofty goal of eradicating Lyme by 2030. “The best chance for making sure no one gets Lyme is to hit it where it lives—in the mice, birds, and ticks in the wild,” says Dr. Hu, who is co-director of the initiative. His team is testing a bait-delivered drug that targets Lyme in wild mice in Massachusetts, followed by sites in other states, to have all key target areas covered within the next five years.
And progress for one chronic illness means progress for others. Long COVID patients are being treated with many of the same interventions that have worked for persistent Lyme symptoms. The similarities in how these diseases impact the immune system are becoming evident, Dr. Kelley says. “The patient awareness and advocacy will continue to grow from here,” she says. “We’re going to see new preventive measures to help people get their lives back faster.”One-on-one connections with people with a persistent illness (Lyme, long COVID, MS, you name it) can be a saving grace, adds Niziol. She exchanged DMs via Instagram with people who helped her find podcasts and advocacy groups. Months into treatment, Niziol is pushing herself to stay active again and remains optimistic. “I’m not going to ignore the hard parts or minimize them,” she says. “But with more understanding, more empathy, there is hope.” Right on.
This article originally appeared in the July/August 2022 issue of Women’s Health.